Articular Cartilage Defect Surgeon

Are you experiencing knee pain and swelling with activity? If so, you may have an articular cartilage defect. Articular cartilage defects occur when cartilage of the knee becomes damaged and can eventually lead to osteoarthritis. Cartilage surgeon, Dr. Jeff Padalecki provides diagnosis and both surgical and nonsurgical treatment options for patients in Austin who have developed an articular cartilage defect. Contact Dr. Padalecki’s team today!
What is Articular Cartilage Defect Surgery?
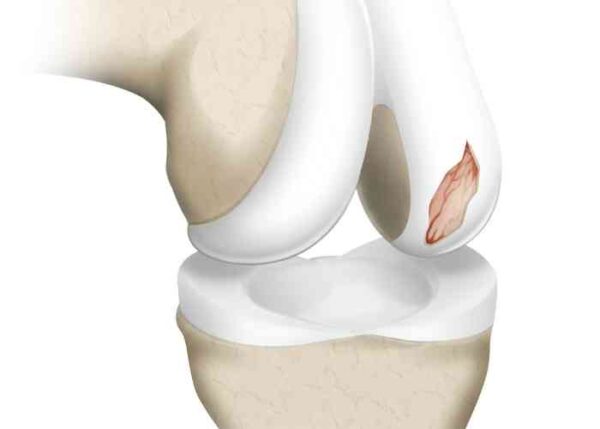
Articular cartilage is a very important component of a healthy knee joint. It covers the ends of each of the bones and allows for a fluid, smooth, painless motion of the knee. When an area of the cartilage becomes damaged, a patient will experience swelling and pain with activities, and over time, this process will continue to progress which eventually leads to complete loss of cartilage down to the bone. When this happens, a diseases known as osteoarthritis becomes present. This continues to cause progressive symptoms of knee pain and stiffness.
When a patient presents damage to the articular cartilage, or an articular cartilage defect, it is of the utmost importance to treat this appropriately in an effort to restore the damaged area and preserve the surrounding cartilage. This treatment will depend on many factors including size of the defect, depth, location, associated injuries in the knee, age, and activity goals. In many cases of a focal cartilage defect, an articular cartilage defect surgery, such as chondroplasty or Microfracture, is recommended by Dr. Jeff Padalecki, Austin, Round Rock, and Cedar Park, Texas communities knee surgeon.
Are you a candidate for articular cartilage defect surgery?
There are two ways to initiate a consultation with Dr. Padalecki:
You can provide current X-rays and/or MRIs for a clinical case review with Dr. Padalecki.
You can schedule an office consultation with Dr. Padalecki.
How is Articular Cartilage Defect Surgery Performed?
There are a variety of surgical procedures that can be used to treat articular cartilage damage. These include chondroplasty, Microfracture, osteochondral autograft transfer, or osteochondral allograft transplantation. Listed below are some of the specific behind each technique:
- Chondroplasty is an arthroscopic procedure used on some patients which involves using a camera and small instruments to trim away the damaged area of cartilage to alleviate the patient’s symptoms and prevent further propagation of the defect. This procedure is typically undertaken in patients who do not have full thickness defects (down to bone).
- Microfracture is a technique used in patients who have a full thickens loss of cartilage. It is a technique where a small pick is used to make holes in the bony surface of the defect. This allows the flow of marrow elements and stem cells which form a clot over the defect and eventually cover the area with a fibrocartilage layer.
- Osteochondral autograft transfer and osteochondral allograft transplantations are two types of procedures where an autograft (taken from the patient) or allograft (taken from a donor) is used. In autograft OATs, small plugs of cartilage and bone are taken from another less important area of the patient’s knee and transferred in to fill the defect. In allograft OATs, the cartilage and bone are taken from a donor and also used to fill the defect. These procedures are done with a combination of arthroscopic and open techniques.
How Long is the Recovery After Cartilage Defect Surgery?
Physical therapy will be prescribed following surgery for an articular cartilage defect. Post-operative management varies depending on the specific type of procedure and the severity of the injury. For chondroplasty, patients are typically on crutches for a few days and allowed to weight bear as tolerated with full range of motion. For the other procedures the patient is placed into a brace and weight bearing is protected for 6-8 weeks. Motion may be initially restricted and a continuous passive motion machine (CPM) is also typically used for 6 weeks after surgery.
For additional information on osteoarthritis of the knee, or to schedule an appointment to discuss articular cartilage defect surgery such as chondroplasty or Microfracture, please contact the office of Austin, Texas orthopedic knee surgeon Dr. Jeff Padalecki.